
A review of shoulder injuries in young athletes
Introduction
Participation in youth sports is widespread throughout the United States, and training is increasingly taking place at younger ages and for a greater duration throughout the year (1). It has been estimated that there are two million sports injuries annually in high school athletes, and among throwing athletes, up to 30% of injuries may involve the shoulder and elbow (2). Shoulder injuries in the pediatric population are often the result of overuse. Issues regarding pitch counts, type of pitches thrown, and constant training have become important topics when discussing injury prevention. This article is a review of the current literature surrounding sports induced shoulder pain, with a particular focus on the adolescent population.
Little Leaguer’s Shoulder (LLS)
Proximal humeral epiphysiolysis, more commonly known as LLS, is a painful condition with increasing incidence (3). The condition is an overuse injury that primarily affects throwing athletes between the ages of 11–16 (4). While this injury is most commonly seen in baseball players, the injury has also been found in tennis players, swimmers, gymnasts, volleyball players, and cricket players (5,6).
LLS is caused by repetitive microtrauma to the skeletally immature proximal humerus. Unfossilized cartilage and rapid linear growth with open physes make this area susceptible (7). The mechanics of adolescent athletes may predispose them to this injury, as athletes in this age group have been found to initiate trunk rotation early during the throwing phase. Trunk rotation during the cocking phase of throwing leads to arm hyper-angulation (8). This places an eccentric load on the adductors and internal rotators of the shoulder. During the release, the physis is subsequently challenged with a distracting force. These repetitive distracting and torsional forces cause disruption in the metaphyseal-physeal blood supply, which can lead to widening of the physis. This physeal widening may be considered a Salter-Harris type I fracture of the proximal humeral physis (5).
Patients will typically present with new onset lateral shoulder pain, often after increasing their pitch count or the types of pitches thrown (9). In addition, the patient may experience decreased pitch control and velocity (9). There is some evidence that recent weight gain or out of season pitching can increase risk for LLS (10).
Physical examination findings commonly include tenderness to palpation over the proximal humerus, shoulder weakness in external rotation, and pain with shoulder range of motion (11). In a recent case series by Heyworth et al., out of 95 patients with LLS, 74% displayed tenderness of the proximal humerus, 34% had decreased range of shoulder motion, and 30% showed glenohumeral internal rotation deficit (GIRD) (3).
Although a diagnosis of LLS is usually made based on history and physical exam findings, imaging can be helpful. Bilateral radiographs should be obtained in order to compare the affected and unaffected sides. These radiographs are also beneficial to rule out a more serious physeal injury (9). Radiographic imaging may show physeal widening and sclerotic bony and cystic changes, as well as calcification (Figure 1) (3,12). However, caution should be used in diagnosing LLS based solely on radiographs, as it has been shown that even asymptomatic athletes may reveal the typical radiographic changes associated with LLS (13). MRI is infrequently obtained, but findings will demonstrate a widened physis and increased T2 signal intensity within the physis and metaphysis (10,14). Hatem et al. demonstrated through a small case series that MRI can be diagnostic, referencing a patient with LLS in which the presumed diagnosis was thought to be a rotator cuff tear (15).
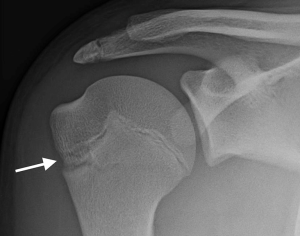
Treatment typically is non-operative, and usually consists of rest and activity modification (4). All throwing activities should be stopped for approximately three months (9). Non-steroidal anti-inflammatory drugs (NSAIDs) may be used to decrease inflammation and pain, and many patients often benefit from physical therapy (3,4). A recent study by Heyworth et al., demonstrated that on average, patients recovered within 2.6 months, with about an additional month or two before resuming competitive sport (3). In case series by Carson et al., 21 of 23 patients (91%) treated with rest for approximately three months had full return to baseball and were asymptomatic (11).
Although prognosis for recovery from LLS is excellent, the primary goal should be aimed at prevention. This is a multifactorial process, and includes coaching proper mechanics, physical conditioning, and limits on pitch counts and year-round participation (4). There are several published guidelines available for specific recommendations on throwing programs and return to play (16,17).
GIRD
Glenohumeral joint kinematics can change in an adaptive manner to chronic overhead activity. This is seen in multiple sports, but especially in baseball, volleyball, handball, and basketball (18-20). All tissues of the shoulder—bone, capsule, and muscle—may be involved (21). During normal human development the humeral head rotates from a retroverted position at birth to an anteverted position as an adult. However, when individuals begin overhead throwing at an early age, extrinsic forces on the humerus cause the humeral head to remain in relative retroversion compared to that of the non-dominant arm. This, combined with tightness of the posteroinferior capsule from chronic reactive scarring, and with scapular dyskinesis with its associated muscular adaptations, creates the constellation of mechanical changes seen in GIRD (21-23).
GIRD has been linked to shoulder pathology that ranges from anterior and superolateral shoulder pain to dead arm syndrome with shoulder instability (23,24). This association has recently been implicated in controversy, as a decrease in shoulder external rotation has also been found to be a predictor of injury (25-27). GIRD has been shown to affect players of all age groups with some evidence for progression as level of competition increases (28-30). In a study of the effect of GIRD in high school baseball players, Lee et al. demonstrated an incidence of GIRD of 21.4% in 56 individuals, which was associated with reduced isokinetic shoulder strength, higher frequency of shoulder pain, and decreased quality of life (31).
A diagnosis of GIRD is based on physical examination of shoulder motion. One method to examine patients involves positioning the patient supine. The arm is abducted to 90 degrees and internal and external rotation are measured up until the point of scapular shift on the thoracic wall (23). Definition of what constitutes GIRD has evolved over the course of the past two decades and is approximately defined at 20 degrees of internal rotational deficit compared to the contralateral arm (21). Moreover, though gain of external rotation in GIRD is more often than not sufficient to allow the total arc of motion to remain equal and circumvent injury, deficits in total arc of motion (TAM or TROM) of greater than 5 degrees compared side-to-side has been implicated in injury (21,24). Hibberd et al. demonstrated that GIRD in youth and adolescent baseball players occurs primarily as a result of humeral retroversion rather than soft tissue tightness in an ultrasound study of 287 individuals of age 6 to 18 years (30). This suggests that early development of GIRD may differ from the pathological GIRD seen in adults that significantly involves soft tissue injury.
Studies show that the magnitude of GIRD and TROM deficits can change acutely following repetitive throwing exposure (21,32). This illustrates soft tissue involvement shifts its arcs of motion, demonstrating that dynamic stabilizers of the shoulder play an important role in prevention of injury as they safeguard the GIRD-affected shoulder from extremes of motion. Fatigue can thus predispose significantly to soft tissue injuries such as thrower’s superior labral tear from anterior to posterior (SLAP) lesions and impingement (33). As such, training programs should not neglect rest and strengthening as part of the therapy regimen (22).
Prevention and treatment of GIRD-related shoulder pathology conventionally begins with stretching exercises but a systematic review of randomized controlled trials on the effectiveness of stretching programs on posterior shoulder tightness and GIRD demonstrated that the sleeper stretch alone is no more effective than no intervention, while increasing evidence supports the use of the passive cross-body stretch in improving GIRD (34). The same study included analyses of combined stretching interventions that showed limited evidence in support of combined active stretching programs (cross-body stretch, sleeper stretch, and overhead stretches) in improving shoulder range of motion. Recent evidence has demonstrated a role for adjunct manual therapy and massage techniques in improving ROM of GIRD-affected shoulders (35-37). Although available data has demonstrated positive effects using passive exercises for treatment of GIRD, there is limited evidence correlating these exercises with ultimate injury prevention.
Effect of various pitch types
Literature demonstrates that pitch types (fastball, curveball, change-up, slider) generally have similar kinematics with only minor differences in forearm and wrist action, and even fewer in the elbow and shoulder (38-42). Fleisig et al. performed a kinematic study involving 21 collegiate baseball pitchers demonstrating the change-up pitch is the least stressful, while the curveball and fastball have similar elbow and shoulder kinetics, with the curveball exhibiting increased forearm supination and radial to ulnar wrist motion (42,43). The authors concluded that no obvious source of injury could be identified from kinematic comparisons between pitches alone. However, a larger prospective cohort study of young baseball players of average age of 12 years demonstrated a statistically significant association of curveball with shoulder pain and slider with elbow pain, suggesting possible age group differences in their vulnerability to breaking pitches (44). Though benefits may be drawn from learning proper pitch mechanics and minimizing breaking pitches, it is likely that adhering to pitch count recommendations far outweighs these benefits in injury prevention (45).
Limited research exists on the biomechanical demands of the softball fast-pitch, as the windmill pitch is regarded as a less stressful motion as compared to the baseball pitch (46). Biomechanically, softball pitches are fundamentally different than that of baseball pitches. Rather than the asymmetrical shoulder range of motion seen in baseball players after training, Softball pitchers have symmetrical findings bilaterally, and have greater strength in the dominant supraspinatus and scapular muscles (middle and lower trapezius) (47). Corben et al. recruited nineteen softball pitchers of an average age of 15.2, and demonstrated greatest degree of asymmetrical fatigue in elbow extension, forearm supination, and shoulder adduction in the throwing arm (47). Elbow flexion was also found to have a higher degree of fatigue, which corroborate with prior EMG findings that showed the biceps brachii muscle activity being twice as high in a windmill pitch as that during the baseball pitch (48). These findings correlate with the relatively high incidence of anterior shoulder pain and overuse rotator cuff injury seen in softball pitchers (48), which should guide injury prevention methods in softball pitchers. Moreover, no such enforcement of pitch count limits currently exists in softball, which can limit efforts in injury prevention.
Monitoring of pitch counts
Pitching injuries have become a focus for concern among junior and adolescent baseball players, with epidemiologic studies demonstrating elbow pain in up to 58% and shoulder pain up to 35% in youth and adolescent baseball players (49). The musculoskeletal adaptations in baseball pitching include GIRD, gain of external rotation, and increased posterior shoulder tightness (50). Musculoskeletal adaptations include stronger internal rotators, external rotators, latissimus dorsi, middle trapezius, and lower trapezius muscles of the dominant versus the non-dominant arm, with no significant difference in the rhomboid and supraspinatus muscles (51). While these observed adaptations differ drastically between the dominant and non-dominant upper extremities of adolescent baseball players, these adaptations alone do not appear to directly predict injury (52).
Enforcement of pitch counts should be foremost in injury prevention. In a case-control study by Olsen et al. in 2006, in which 95 adolescent pitchers who had shoulder or elbow surgery were compared to 45 controls, it was found that the injured group pitched significantly more games per year, innings per game, and had higher pitch counts during and before games (53). Interestingly, no differences were found regarding exercise programs, stretching practices, relieving frequency, pitch type frequency. Erickson et al. demonstrated that exceeding pitch count recommendations in Little League baseball can increase the chance of requiring ulnar collateral ligament reconstruction surgery in later career (54). Of a total of 62 Little League World Series pitchers that progressed to professional play, 4 exceeded pitch counts, and of these, 50% required ulnar collateral ligament reconstruction, versus only 1.7% in those who did not exceed pitch counts (54). In a survey study of 95 Little League coaches, knowledge of pitching recommendations for young pitchers was found to be poor, with only 35% to 62% of the pitching guideline questions were answered correctly. Furthermore, only 73% of coaches state that they follow pitching guidelines, and 29% allowed their pitchers to throw breaking pitches (55). Pitch count violations tend to increase with age (56), while the degree of pitch recommendation enforcement from coaches concurrently decreases (55). These findings support the correlation of shoulder and elbow overuse in youth and adolescent baseball and injury.
Shoulder injuries in volleyball
Volleyball is a popular international sport with a relatively healthy injury profile for the shoulder, which only accounted for 17 of 193 body part injuries out of 10,621 hours played in one epidemiological study of junior world-class volleyball (57). Majority of injuries resulted from the ankle, followed by the knee, the hand, and the lower back (57,58). Shoulder pain, however, appears to be a prevalent concern among young volleyball players (59,60). GIRD-associated shoulder pathology has also been implicated in volleyball in a similar fashion as in baseball, but is less well studied and does not consistently correlate to shoulder problems.
Within the smaller cohort of volleyball-associated shoulder injuries, the rotator cuff appears to play a larger role in pathology (61-63). Harput et al. demonstrated a statistically significant decrease in the acromiohumeral distance in the dominant shoulder of adolescent volleyball attackers compared to the non-dominant shoulder suggesting increased potential for rotator cuff impingement (63). Infraspinatus syndrome presenting as weakness of the infraspinatus muscle secondary to injury to the suprascapular nerve also appears to be prevalent in volleyball, and one kinematic study suggests that greater shoulder abduction and horizontal adduction at the moment of ball strike may contribute to traction-related injury to the suprascapular nerve (64). Electromyography (EMG) and nerve conduction tests corroborate these findings in professional beach volleyball players, with prevalence of infraspinatus atrophy reported to be as high as 34% (65).
Injury prevention for the volleyball shoulder should primarily focus on minimizing excessive force on the rotator cuff and glenohumeral joint. For instance, Seminati et al. showed that an alternative technique to volleyball spike may be less traumatic to the rotator cuff as compared to the traditional spike technique by decreasing shoulder adduction in favor of forward elevation (66). A randomized controlled trial performed on university volleyball, swimming, and tennis players demonstrated that sleeper stretching improves dominant shoulder internal rotation and horizontal adduction at 8 weeks’ follow-up (67). Gouttebarge et al. performed a systematic development of an injury prevention intervention for volleyball using evidence-based multidisciplinary meetings to identify key exercises to comprise a therapy program (68). The 15-minute program comprehensively focused on full-body on-court exercises and stretches for injury prevention in the ankles, knees, hands, wrists, and shoulders. Though deemed too demanding as a pre-game warm-up routine, such programs can be integrated into training schedules and create grounds for improving injury prevention awareness (68).
Quadrilateral space syndrome (QSS)
QSS is an uncommon process that can manifest in several ways, and it was recently proposed by Brown et al. that this syndrome has two separate entities, vascular QSS (vQSS), affecting the posterior circumflex humeral artery (PCHA), and neurogenic QSS (nQSS), affecting the axillary nerve. QSS is most often seen in overhead athletes, including swimmers as well as baseball, tennis, and volleyball players (69). However, the symptoms can present in any patient who conducts repetitive overhead movement, such as window cleaners or yoga participants (70).
The quadrilateral space is an anatomic area bounded by the long head of the triceps medially, the medial edge of the surgical neck of the humerus laterally, the teres major and latissimus dorsi inferiorly, and the teres minor or glenohumeral joint capsule superiorly. Overhead athletes typically have a history of repetitive abduction and external rotation movements of the arm, which can lead to compression or mechanical injury to the contents of the quadrilateral space. It has been estimated that nerve symptoms are more common than vascular symptoms, with a ratio of 1.5:1 (70). Overall, there is a predilection for males over females, with a ratio of 7:1 respectively (70). This is likely due to the increased prevalence of overhead activities in male dominated sports, such as baseball (70).
Compression of the PCHA (vQSS) can cause localized thrombosis and aneurysm formation, sometimes leading to emboli that can lead to symptoms distally in the extremity. The ischemia caused by these thrombi can manifest with pain, absent pulses, coolness, and pallor of the affected hand or digit (70). Differential diagnosis in the adolescent population may include thoracic outlet syndrome, hypothenar hammer syndrome, and autoimmune conditions such as vasculitis or scleroderma. Diagnostic imaging can be of significant value, with the use of digital subtraction angiography (DSA), CT angiography, and MR angiography being able to identify a thrombus or aneurysm of the PCHA. DSA may be particularly beneficial; in addition to diagnostic value, it can be used therapeutically for thrombolysis (70). Surgical treatment may be necessary, and often involves ligation of the PCHA in order to prevent distal embolization (70).
Neurogenic QSS has a different presentation than vQSS. The irritation of the axillary nerve is commonly attributed to fibrous bands that develop from repetitive trauma to the soft tissue within the quadrilateral space (71). Paralabral cysts have also been reported as a cause of QSS (72). Symptoms are typically varied, but often include pain over the posterior shoulder, neuropathic pain that may nondermatomal, shoulder numbness, shoulder weakness, and radiating pain (70). Differential diagnosis should include complex regional pain syndrome, suprascapular nerve entrapment, rotator cuff syndrome, and C5-C6 radiculopathy (69,70). Diagnostic imaging such as MRI has been shown help to establish a diagnosis by highlighting isolated teres minor weakness (73). However, several studies have called into question whether isolated teres minor denervation as seen on MRI is associated with QSS (74,75). EMG and nerve conduction studies (NCS) have been shown to have non-specific results (69).
Initial treatment for this QSS includes activity modification, physical therapy, and non-steroidal anti-inflammatory medications. However, in high level athletes who wish to remain engaged in their sport of choice, avoiding shoulder abduction and external rotation may not be realistic. Patients who fail conservative management often require surgery, which includes neurolysis and excision of fibrous bands or any other space-occupying lesion near the axillary nerve (70).
After surgery for vQSS or nQSS, patients are typically able to return to sport after several weeks, often with complete resolution of symptoms and no shoulder deficits (76). QSS is an uncommon source of shoulder and upper extremity pain, and other diagnoses must be excluded. Nevertheless, the treating physician should maintain a high index of suspicion for QSS in overhead athletes who present with neurogenic or vascular symptoms in the presence of shoulder pain.
Dislocation
Shoulder dislocation events are relatively rare in non-contact overhead sports in the young athlete (77). The extent of bony injury also tends to be less in non-contact overhead sports as compared to contact sports (78). However, if a first-time dislocation does occur, primary reduction of the shoulder should be performed in a controlled manner. Consideration should be given to the physically fit young athlete in the closed reduction of the shoulder injury; due to increased muscle mass, it is advisable to have a low threshold for premedication with sedation, intravenous and/or intra-articular analgesia prior to reduction to minimize additional injuries to the bone or soft tissue (79).
Traditionally, immobilization for 6 weeks in a sling in internal rotation with gradual out of sling exercises, followed by at least 4 weeks of physical therapy has been the treatment of choice for first-time dislocators (80). In cases without extensive tissue injury and with diligent rehabilitation, athletes can in some instances return to play as early as 3 weeks after injury (81). Recently however, there has been an increased trend in arthroscopic stabilization of first-time shoulder dislocators, especially in younger skeletally-mature patients and athletes at the end of the sporting season, as a result of the findings from a number of non-blinded randomized trials demonstrating its efficacy in preventing future instability events (79,80,82,83). This may be of additional pertinence to the overhead athlete for whom the mechanics of their overhead activity may predispose them to further instability events. Contrarily, the limited data that exists on that of skeletally immature patients who underwent operative versus non-operative therapy for first-time shoulder dislocation demonstrate a tendency for operative patients to do worse (84,85). Overall, current literature supports consideration for surgical intervention in first-time dislocation in the skeletally mature young overhead athlete, and in recurrent dislocation in the skeletally immature patient.
Hypermobility (JH)
JH, which is diagnosed when a joint has an exaggerated range of motion, may present in several ways and is involved in a variety of conditions. Joint hypermobility syndrome (JHS) is when the joint has increased range of motion in conjunction with musculoskeletal pain (86,87). This entity can exist in conditions such as generalized JHS, benign JHS, and Ehlers-Danlos syndrome (hypermobile type) (86,88,89). Children with JHS may complain of cramps in their leg muscles, especially at night (88). It may also be associated with generalized pain, fibromyalgia, musculoskeletal injuries, and anxiety (86). Conversely, El-Metwally et al. demonstrated that in Finnish adolescents, hypermobility was not predictive of future musculoskeletal pain, either traumatic or atraumatic in nature. However, follow up in this study was only 1 year, which limits its prognostic value considerably (90).
A common measurement of hypermobility is the Beighton score, a well-known criterion that measures mobility of several joints, including the hands, elbows, knees, and trunk (88). Smits-Engelsman et al. have validated this criterion in children, and noted that a higher Beighton score corresponds to increased range of motion even in joints that are not measured as part of the criteria. In their cohort of Dutch elementary school students, 35% scored 6/9 or greater on the Beighton score, which is considered hypermobile (87). It has also been described that swimmers, ballet dancers, gymnasts, and musicians have a higher prevalence of JHS (86). Hypermobility itself is not a pathology; it is only diagnosed as a syndrome when the patient is in pain due to their laxity.
Generalized JHS may specifically affect the shoulder, and this may lead to increased incidence of musculoskeletal symptoms in the head and neck area (86). In one recent study of a Danish cohort, generalized joint hypermobility was found to be prevalent in 30% of the population, while generalized joint hypermobility of the shoulder was only 5% (86). In addition, there is a high prevalence of generalized hyperlaxity in patients who have shoulder multidirectional instability (91).
JHS may be a hereditary condition (86). Em et al. showed that the enzyme prolidase, involved in collagen formation and degradation, is significantly lower in patients with benign JHS (89). Regardless of etiology, this is a disease that is best treated conservatively, and there is evidence that exercises and physical therapy can help reduce painful symptoms associated with joint hypermobility (92).
Conclusions
There are a variety of shoulder injuries that can affect the young athlete, and because of the open physes in the pediatric population, overuse injuries are of critical concern. It is therefore important to educate parents, coaches, and athletes about the danger of overusing the shoulder. In addition to the conditions described in this article, children and adolescents, like adults, can suffer rotator cuff tears, labral tears, and instability episodes from athletic play. The management of such injuries is beyond the scope of this focused article, yet these conditions are nonetheless important diagnostic considerations in a young athlete with shoulder pain. Although most pediatric shoulder injuries can be treated non-operatively with therapy and rest, some, such as QSS, may require surgery. During examination of all pediatric musculoskeletal complaints, global issues such as hypermobility must also be assessed. A multidisciplinary approach with emphasis on proper training is vital to the prevention and treatment of these injuries.
Acknowledgments
We would like to give thanks to Dr. Sheena Ranade for providing clinical imaging for this manuscript. We also give thanks to Carolyn Kushner, for her assistance in the submission process of this work.
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned by the Guest Editors (Alexis Chiang Colvin and Diana Patterson) for the series “Orthopaedic Sports Injuries in Youth” published in Annals of Joint. The article has undergone external peer review.
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/aoj.2018.02.04). The series “Orthopaedic Sports Injuries in Youth” was commissioned by the editorial office without any funding or sponsorship. The authors have no other conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Wu M, Fallon R, Heyworth BE. Overuse Injuries in the Pediatric Population. Sports Med Arthrosc 2016;24:150-8. [Crossref] [PubMed]
- Smucny M, Kolmodin J, Saluan P. Shoulder and Elbow Injuries in the Adolescent Athlete. Sports Med Arthrosc 2016;24:188-94. [Crossref] [PubMed]
- Heyworth BE, Kramer DE, Martin DJ, et al. Trends in the Presentation, Management, and Outcomes of Little League Shoulder. Am J Sports Med 2016;44:1431-8. [Crossref] [PubMed]
- Osbahr DC, Kim HJ, Dugas JR. Little league shoulder. Curr Opin Pediatr 2010;22:35-40. [Crossref] [PubMed]
- Paz DA, Chang GH, Yetto JM Jr, et al. Upper extremity overuse injuries in pediatric athletes: clinical presentation, imaging findings, and treatment. Clin Imaging 2015;39:954-64. [Crossref] [PubMed]
- Drescher WR, Falliner A, Zantop T, et al. Little league shoulder syndrome in an adolescent cricket player. Br J Sports Med 2004;38:E14 [Crossref] [PubMed]
- Marshall KW. Overuse upper extremity injuries in the skeletally immature patient: beyond Little League shoulder and elbow. Semin Musculoskelet Radiol 2014;18:469-77. [Crossref] [PubMed]
- Keeley DW, Hackett T, Keirns M, et al. A biomechanical analysis of youth pitching mechanics. J Pediatr Orthop 2008;28:452-9. [Crossref] [PubMed]
- Brennan BW, Kelly MJ. Little Leaguer's Shoulder. Clinical Pediatrics 2011;50:462-3. [Crossref] [PubMed]
- Davis KW. Imaging Pediatric Sports Injuries: Upper Extremity. Radiol Clin North Am 2010;48:1199-211. [Crossref] [PubMed]
- Carson WG Jr, Gasser SI. Little Leaguer's shoulder. A report of 23 cases. Am J Sports Med 1998;26:575-80. [Crossref] [PubMed]
- Anton C, Podberesky DJ. Little League shoulder: a growth plate injury. Pediatr Radiol 2010;40:S54. [Crossref] [PubMed]
- Murachovsky J, Ikemoto RY, Nascimento LG, et al. Does the presence of proximal humerus growth plate changes in young baseball pitchers happen only in symptomatic athletes? An x ray evaluation of 21 young baseball pitchers. Br J Sports Med 2010;44:90-4. [Crossref] [PubMed]
- Song JC, Lazarus ML, Song AP. MRI findings in Little Leaguer's shoulder. Skeletal Radiol 2006;35:107-9. [Crossref] [PubMed]
- Hatem SF, Recht MP, Profitt B. MRI of Little Leaguer's shoulder. Skeletal Radiol 2006;35:103-6. [Crossref] [PubMed]
- Axe MJ, Snyder-Mackler L, Konin JG, et al. Development of a distance-based interval throwing program for Little League-aged athletes. Am J Sports Med 1996;24:594-602. [Crossref] [PubMed]
- Reinold MM, Wilk KE, Reed J, et al. Interval sport programs: guidelines for baseball, tennis, and golf. J Orthop Sports Phys Ther 2002;32:293-8. [Crossref] [PubMed]
- Hibberd EE, Oyama S, Tatman J, et al. Dominant-limb range-of-motion and humeral-retrotorsion adaptation in collegiate baseball and softball position players. J Athl Train 2014;49:507-13. [Crossref] [PubMed]
- Seabra P, Van Eck CF, Sa M, et al. Are professional handball players at risk for developing a glenohumeral internal rotation deficit in their dominant arm? Phys Sportsmed 2017;45:77-81. [PubMed]
- Guney H, Harput G, Colakoglu F, et al. The Effect of Glenohumeral Internal-Rotation Deficit on Functional Rotator-Strength Ratio in Adolescent Overhead Athletes. J Sport Rehabil 2016;25:52-7. [Crossref] [PubMed]
- Kibler WB, Sciascia A, Thomas SJ. Glenohumeral internal rotation deficit: pathogenesis and response to acute throwing. Sports Med Arthrosc 2012;20:34-8. [Crossref] [PubMed]
- Burkhart SS, Morgan CD, Kibler WB. The disabled throwing shoulder: spectrum of pathology Part III: The SICK scapula, scapular dyskinesis, the kinetic chain, and rehabilitation. Arthroscopy 2003;19:641-61. [Crossref] [PubMed]
- Burkhart SS, Morgan CD, Kibler WB. The disabled throwing shoulder: spectrum of pathology Part I: pathoanatomy and biomechanics. Arthroscopy 2003;19:404-20. [Crossref] [PubMed]
- Wilk KE, Macrina LC, Fleisig GS, et al. Correlation of glenohumeral internal rotation deficit and total rotational motion to shoulder injuries in professional baseball pitchers. Am J Sports Med 2011;39:329-35. [Crossref] [PubMed]
- Wilk KE, Macrina LC, Fleisig GS, et al. Deficits in Glenohumeral Passive Range of Motion Increase Risk of Shoulder Injury in Professional Baseball Pitchers: A Prospective Study. Am J Sports Med 2015;43:2379-85. [Crossref] [PubMed]
- Manske R, Wilk KE, Davies G, et al. Glenohumeral motion deficits: friend or foe? Int J Sports Phys Ther 2013;8:537-53. [PubMed]
- Camp CL, Zajac JM, Pearson DB, et al. Decreased Shoulder External Rotation and Flexion Are Greater Predictors of Injury Than Internal Rotation Deficits: Analysis of 132 Pitcher-Seasons in Professional Baseball. Arthroscopy 2017;33:1629-36. [Crossref] [PubMed]
- Nakamizo H, Nakamura Y, Nobuhara K, et al. Loss of glenohumeral internal rotation in little league pitchers: a biomechanical study. J Shoulder Elbow Surg 2008;17:795-801. [Crossref] [PubMed]
- Kar S, Bretherton-Watt D, Gibson SJ, et al. Novel peptide pancreastatin: its occurrence and codistribution with chromogranin A in the central nervous system of the pig. J Comp Neurol 1989;288:627-39. [Crossref] [PubMed]
- Hibberd EE, Oyama S, Myers JB. Increase in humeral retrotorsion accounts for age-related increase in glenohumeral internal rotation deficit in youth and adolescent baseball players. Am J Sports Med 2014;42:851-8. [Crossref] [PubMed]
- Lee J, Kim LN, Song H, et al. The effect of glenohumeral internal rotation deficit on the isokinetic strength, pain, and quality of life in male high school baseball players. Ann Rehabil Med 2015;39:183-90. [Crossref] [PubMed]
- Reinold MM, Wilk KE, Macrina LC, et al. Changes in shoulder and elbow passive range of motion after pitching in professional baseball players. Am J Sports Med 2008;36:523-7. [Crossref] [PubMed]
- Burkhart SS, Morgan CD, Kibler WB. The disabled throwing shoulder: spectrum of pathology. Part II: evaluation and treatment of SLAP lesions in throwers. Arthroscopy 2003;19:531-9. [Crossref] [PubMed]
- Mine K, Nakayama T, Milanese S, et al. Effectiveness of Stretching on Posterior Shoulder Tightness and Glenohumeral Internal-Rotation Deficit: A Systematic Review of Randomized Controlled Trials. J Sport Rehabil 2017;26:294-305. [Crossref] [PubMed]
- Bailey LB, Thigpen CA, Hawkins RJ, et al. Effectiveness of Manual Therapy and Stretching for Baseball Players With Shoulder Range of Motion Deficits. Sports Health 2017;9:230-7. [Crossref] [PubMed]
- Fairall RR, Cabell L, Boergers RJ, et al. Acute effects of self-myofascial release and stretching in overhead athletes with GIRD. J Bodyw Mov Ther 2017;21:648-52. [Crossref] [PubMed]
- Yang JL, Chen SY, Hsieh CL, et al. Effects and predictors of shoulder muscle massage for patients with posterior shoulder tightness. BMC Musculoskelet Disord 2012;13:46. [Crossref] [PubMed]
- Sakurai S, Ikegami Y, Okamoto A, et al. A three dimensional cinematographic analysis of upper limb movement during fastball and curveball pitches. J Appl Biomech 1993;9:47-65. [Crossref]
- Barrentine S, Matsuo T, Escamilla R, et al. Kinematic analysis of the wrist and forearm during baseball pitching. J Appl Biomech 1998;14:24-39. [Crossref]
- Elliott B, Grove J. A three-dimensional cinematographic analysis of the fastball and curveball pitches in baseball. Int J Sports Biomech 1986;2:20-8. [Crossref]
- Escamilla RF, Fleisig GS, Barrentine SW, et al. Kinematic comparisons of throwing different types of baseball pitches. J Appl Biomech 1998;14:1-23. [Crossref]
- Fleisig GS, Kingsley DS, Loftice JW, et al. Kinetic comparison among the fastball, curveball, change-up, and slider in collegiate baseball pitchers. Am J Sports Med 2006;34:423-30. [Crossref] [PubMed]
- Nissen CW, Westwell M, Ounpuu S, et al. A biomechanical comparison of the fastball and curveball in adolescent baseball pitchers. Am J Sports Med 2009;37:1492-8. [Crossref] [PubMed]
- Lyman S, Fleisig GS, Andrews JR, et al. Effect of pitch type, pitch count, and pitching mechanics on risk of elbow and shoulder pain in youth baseball pitchers. Am J Sports Med 2002;30:463-8. [Crossref] [PubMed]
- Henriksson C, Aldenborg F, Haljamae H, et al. Renal cell carcinoma with vena cava extension: diagnostic and surgical features of 41 cases. Scand J Urol Nephrol 1987;21:291-6. [Crossref] [PubMed]
- Loosli AR, Requa RK, Garrick JG, et al. Injuries to pitchers in women's collegiate fast-pitch softball. Am J Sports Med 1992;20:35-7. [Crossref] [PubMed]
- Corben JS, Cerrone SA, Soviero JE, et al. Performance Demands in Softball Pitching: A Comprehensive Muscle Fatigue Study. Am J Sports Med 2015;43:2035-41. [Crossref] [PubMed]
- Rojas IL, Provencher MT, Bhatia S, et al. Biceps activity during windmill softball pitching: injury implications and comparison with overhand throwing. Am J Sports Med 2009;37:558-65. [Crossref] [PubMed]
- Dun S, Loftice J, Fleisig GS, et al. A biomechanical comparison of youth baseball pitches: is the curveball potentially harmful? Am J Sports Med 2008;36:686-92. [Crossref] [PubMed]
- McHugh MP, Tyler TF, Mullaney MJ, et al. The Effect of a High Pitch Volume on Musculoskeletal Adaptations in High School Baseball Pitchers. Am J Sports Med 2016;44:2246-54. [Crossref] [PubMed]
- Trakis JE, McHugh MP, Caracciolo PA, et al. Muscle strength and range of motion in adolescent pitchers with throwing-related pain: implications for injury prevention. Am J Sports Med 2008;36:2173-8. [Crossref] [PubMed]
- Oyama S, Hibberd EE, Myers JB. Preseason screening of shoulder range of motion and humeral retrotorsion does not predict injury in high school baseball players. J Shoulder Elbow Surg 2017;26:1182-9. [Crossref] [PubMed]
- Olsen SJ 2nd, Fleisig GS, Dun S, et al. Risk factors for shoulder and elbow injuries in adolescent baseball pitchers. Am J Sports Med 2006;34:905-12. [Crossref] [PubMed]
- Erickson BJ, Chalmers PN, Axe MJ, et al. Exceeding Pitch Count Recommendations in Little League Baseball Increases the Chance of Requiring Tommy John Surgery as a Professional Baseball Pitcher. Orthop J Sports Med 2017;5:2325967117695085 [Crossref] [PubMed]
- Dupoisot H, Bouchet H, Laoussad S, et al. Chronorhythms of the circulating erythrocytes and leukocytes--correlation with the E.S.R. cycles. Chronobiol Int 1987;4:499-508. [Crossref] [PubMed]
- Riff AJ, Chalmers PN, Sgroi T, et al. Epidemiologic Comparison of Pitching Mechanics, Pitch Type, and Pitch Counts Among Healthy Pitchers at Various Levels of Youth Competition. Arthroscopy 2016;32:1559-68. [Crossref] [PubMed]
- Bere T, Kruczynski J, Veintimilla N, et al. Injury risk is low among world-class volleyball players: 4-year data from the FIVB Injury Surveillance System. Br J Sports Med 2015;49:1132-7. [Crossref] [PubMed]
- Reeser JC, Gregory A, Berg RL, et al. A Comparison of Women's Collegiate and Girls' High School Volleyball Injury Data Collected Prospectively Over a 4-Year Period. Sports Health 2015;7:504-10. [Crossref] [PubMed]
- Frisch KE, Clark J, Hanson C, et al. High Prevalence of Nontraumatic Shoulder Pain in a Regional Sample of Female High School Volleyball Athletes. Orthop J Sports Med 2017;5:2325967117712236 [Crossref] [PubMed]
- Forthomme B, Wieczorek V, Frisch A, et al. Shoulder pain among high-level volleyball players and preseason features. Med Sci Sports Exerc 2013;45:1852-60. [Crossref] [PubMed]
- Mach U, Puzyna W. Hemorrhage in the early puerperium in a carrier of the hemophilia B gene. Ginekol Pol 1987;58:636-40. [PubMed]
- Seminati E, Minetti AE. Overuse in volleyball training/practice: A review on shoulder and spine-related injuries. Eur J Sport Sci 2013;13:732-43. [Crossref] [PubMed]
- Harput G, Guney H, Toprak U, et al. Shoulder-Rotator Strength, Range of Motion, and Acromiohumeral Distance in Asymptomatic Adolescent Volleyball Attackers. J Athl Train 2016;51:733-8. [Crossref] [PubMed]
- Reeser JC, Fleisig GS, Cools AM, et al. Biomechanical insights into the aetiology of infraspinatus syndrome. Br J Sports Med 2013;47:239-44. [Crossref] [PubMed]
- Lajtai G, Wieser K, Ofner M, et al. Electromyography and nerve conduction velocity for the evaluation of the infraspinatus muscle and the suprascapular nerve in professional beach volleyball players. Am J Sports Med 2012;40:2303-8. [Crossref] [PubMed]
- Seminati E, Marzari A, Vacondio O, et al. Shoulder 3D range of motion and humerus rotation in two volleyball spike techniques: injury prevention and performance. Sports Biomech 2015;14:216-31. [Crossref] [PubMed]
- Chepeha JC, Magee DJ, Bouliane M, et al. Effectiveness of a Posterior Shoulder Stretching Program on University-Level Overhead Athletes: Randomized Controlled Trial. Clin J Sport Med 2017; [Epub ahead of print]. [Crossref] [PubMed]
- Gouttebarge V, van Sluis M, Verhagen E, et al. The prevention of musculoskeletal injuries in volleyball: the systematic development of an intervention and its feasibility. Inj Epidemiol 2017;4:25. [Crossref] [PubMed]
- Hoskins WT, Pollard HP, McDonald AJ. Quadrilateral space syndrome: a case study and review of the literature. Br J Sports Med 2005;39:e9 [Crossref] [PubMed]
- Brown SA, Doolittle DA, Bohanon CJ, et al. Quadrilateral space syndrome: the Mayo Clinic experience with a new classification system and case series. Mayo Clin Proc 2015;90:382-94. [Crossref] [PubMed]
- Sato T, Tsai TL, Altamimi A, et al. Quadrilateral Space Syndrome: A Case Report. J Hand Surg Asian Pac Vol 2017;22:125-7. [Crossref] [PubMed]
- Sanders TG, Tirman PF. Paralabral cyst: an unusual cause of quadrilateral space syndrome. Arthroscopy 1999;15:632-7. [Crossref] [PubMed]
- Linker CS, Helms CA, Fritz RC. Quadrilateral space syndrome: findings at MR imaging. Radiology 1993;188:675-6. [Crossref] [PubMed]
- Sofka CM, Lin J, Feinberg J, et al. Teres minor denervation on routine magnetic resonance imaging of the shoulder. Skeletal Radiol 2004;33:514-8. [Crossref] [PubMed]
- Wilson L, Sundaram M, Piraino DW, et al. Isolated teres minor atrophy: manifestation of quadrilateral space syndrome or traction injury to the axillary nerve? Orthopedics 2006;29:447-50. [PubMed]
- McAdams TR, Dillingham MF. Surgical decompression of the quadrilateral space in overhead athletes. Am J Sports Med 2008;36:528-32. [Crossref] [PubMed]
- Robinson TW, Corlette J, Collins CL, et al. Shoulder injuries among US high school athletes, 2005/2006-2011/2012. Pediatrics 2014;133:272-9. [Crossref] [PubMed]
- Nakagawa S, Ozaki R, Take Y, et al. Enlargement of Glenoid Defects in Traumatic Anterior Shoulder Instability: Influence of the Number of Recurrences and Type of Sport. Orthop J Sports Med 2014;2:2325967114529920 [Crossref] [PubMed]
- Sedeek SM, Bin Abd Razak HR, Ee GW, et al. First-time anterior shoulder dislocations: should they be arthroscopically stabilised? Singapore Med J 2014;55:511-5; quiz 516. [Crossref] [PubMed]
- Kirkley A, Werstine R, Ratjek A, et al. Prospective randomized clinical trial comparing the effectiveness of immediate arthroscopic stabilization versus immobilization and rehabilitation in first traumatic anterior dislocations of the shoulder: long-term evaluation. Arthroscopy 2005;21:55-63. [Crossref] [PubMed]
- Burns TC, Owens BD. Management of shoulder instability in in-season athletes. Phys Sportsmed 2010;38:55-60. [Crossref] [PubMed]
- Yanmis I, Tunay S, Komurcu M, et al. Outcomes of acute arthroscopic repair and conservative treatment following first traumatic dislocation of the shoulder joint in young patients. Ann Acad Med Singapore 2003;32:824-7. [PubMed]
- Jakobsen BW, Johannsen HV, Suder P, et al. Primary repair versus conservative treatment of first-time traumatic anterior dislocation of the shoulder: a randomized study with 10-year follow-up. Arthroscopy 2007;23:118-23. [Crossref] [PubMed]
- Khan A, Samba A, Pereira B, et al. Anterior dislocation of the shoulder in skeletally immature patients: comparison between non-operative treatment versus open Latarjet's procedure. Bone Joint J 2014;96-B:354-9. [Crossref] [PubMed]
- Cordischi K, Li X, Busconi B. Intermediate outcomes after primary traumatic anterior shoulder dislocation in skeletally immature patients aged 10 to 13 years. Orthopedics 2009;32: [Crossref] [PubMed]
- Juul-Kristensen B, Ostengaard L, Hansen S, et al. Generalised joint hypermobility and shoulder joint hypermobility, - risk of upper body musculoskeletal symptoms and reduced quality of life in the general population. BMC Musculoskelet Disord 2017;18:226. [Crossref] [PubMed]
- Smits-Engelsman B, Klerks M, Kirby A. Beighton Score: A Valid Measure for Generalized Hypermobility in Children. J Pediatr 2011;158:119-23, 123.e1-4.
- Beighton P, Horan FT. Surgical aspects of the Ehlers-Danlos syndrome. A survey of 100 cases. Br J Surg 1969;56:255-9. [Crossref] [PubMed]
- Em S, Ucar D, Oktayoglu P, et al. Serum prolidase activity in benign joint hypermobility syndrome. BMC Musculoskelet Disord 2014;15:75. [Crossref] [PubMed]
- El-Metwally A, Salminen JJ, Auvinen A, et al. Risk factors for development of non-specific musculoskeletal pain in preteens and early adolescents: a prospective 1-year follow-up study. BMC Musculoskelet Disord 2007;8:46. [Crossref] [PubMed]
- Saccomanno MF, Fodale M, Capasso L, et al. Generalized joint laxity and multidirectional instability of the shoulder. Joints 2014;1:171-9. [Crossref] [PubMed]
- Palmer S, Bailey S, Barker L, et al. The effectiveness of therapeutic exercise for joint hypermobility syndrome: a systematic review. Physiotherapy 2014;100:220-7. [Crossref] [PubMed]
Cite this article as: Solomon D, Cong GT, Cagle P. A review of shoulder injuries in young athletes. Ann Joint 2018;3:12.


