
Scapular body fractures—should we be fixing more of these?
Introduction
The question of whether we should be fixing more scapular body fractures originates from the historical preference for nonoperative management of these fractures. Recently, there has been a renewed interest in operative management due to the recognition that scapular malunion can cause significant disability. While the treatment pendulum has shifted away from benign neglect, surgical indications remain controversial.
The concept of surgical fixation for scapula fractures is not novel. The first publication of internal fixation for a scapula fracture was in 1913 by Albin Lambotte from a case performed in 1910 (1). Despite numerous surgical case series from surgeons such as Judet (1), it was the nonoperative opinion of Rowe (2) and Schnepp (3) that dictated how these fractures would be treated for ensuing decades. Nonoperative treatment gained traction due to a few inherent properties of the scapula. First, the robust muscular envelope and bloody supply of the scapula ensure that the majority of these fractures will proceed to union. Additionally, the glenohumeral and scapulothoracic joints maintain a large capacity for compensatory motion if the scapula heals in a malunited position. For these reasons, coupled with the fact that the scapula has complex bony anatomy with little area for screw purchase, nonoperative management was the prevailing treatment until the turn of the twenty first century.
The treatment strategy for these fractures changed as the understanding of the fracture patterns, surgical approaches, fixation technology improved and the consequences of scapular malunion were realized. Initial efforts for operative treatment of scapula fractures largely revolved around intra-articular glenoid fractures due to well accepted principles of restoring articular congruity and preventing post-traumatic osteoarthritis (4). More recently, it has been recognized that certain patients with extra-articular scapula fractures can have poor functional outcomes related to altered rotator cuff biomechanics, scapulothoracic dyskinesia, and impingement syndrome (5).
Even though surgical intervention has become increasingly recognized as appropriate treatment for certain patients, identifying these patients still remains elusive. The recent standardization of radiographic parameters for displacement of scapular body fractures has led to improved guidelines for surgical intervention (6). However, even to this date, high quality evidence comparing nonoperative to operative treatment of scapular body fractures does not exist.
Patient evaluation
Scapula fractures are rare injuries, comprising only about 0.5% of all fractures. However, fractures of the scapular body or glenoid neck account for approximately 66–98% of scapula fractures making them the most common fracture pattern (7).
Scapula fractures are usually the result of high-energy mechanisms and patients frequently have associated injuries. These injuries include thorax, ipsilateral upper extremity, head, and spine injuries in 80%, 50%, 48%, and 26%, respectively (8). Scapula fractures should alert the treating orthopaedic surgeon to the potential presence of these other injuries so they can be treated appropriately. Displaced rib fractures can have a significant effect on the outcome of patients with scapular body fractures due to prominence and irritation to the patient (9). Alternatively, scapular fracture diagnosis can be missed or delayed due to the presence of these more significant injuries. Any patient with multiple rib fractures or hemopneumothorax on a chest radiograph should draw the attention to the scapula to ensure it was not injured.
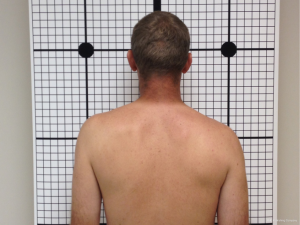
Physical examination of the patient should include gross inspection of the shoulder for significant deformity. This deformity is often characterized by marked shoulder drooping or ptosis on the injured side (Figure 1). The integrity of the skin and assessment for abrasions over the shoulder should be noted. Palpation of the acromion, clavicle and sternoclavicular/acromioclavicular joints can alert the physician to associated fractures that would constitute a double disruption of the shoulder suspensory complex. Range of motion of the shoulder will undoubtedly be painful, but if near full active forward elevation is present it can let the provider know the fracture is likely nondisplaced and can safely be treated conservatively.
If a scapular fracture is identified on a chest radiograph, a standard shoulder radiographic series including true AP shoulder (Grashey), axillary, and scapular Y views to assess for displacement should be obtained. If marked displacement is identified, a dedicated computed tomography scan with 3D reconstructions can help define the displacement indicative of potential surgical benefit.
Classification/radiological evaluation
Numerous classification systems exist for scapular body fractures, most notably including those of Hardegger (4), Ada and Miller (10), as well as the OTA/AO fracture and dislocation classification (11). Both the Hardegger and Ada and Miller classifications were based on radiographic appearance of fracture lines rather than CT scans. These classification systems broadly group fractures into distinct categories such as scapular spine (IB), scapular neck (IIA, B, C), glenoid (III), and body (IV) fractures for the Ada and Miller classification (10). More recently, with the advent of CT scans, detailed mapping of scapular body fractures was able to be performed. Based on a series of ninety patients with operative scapular body fractures, 3-dimensional mapping of the fractures revealed the vast majority of scapular body fractures followed predictable patterns (7). These patterns included a high rate of those with a fracture of the lateral border just inferior to the glenoid, often with extension to the medial border (7). Early classifications systems laid the groundwork for contemporary surgical indications while three-dimensional mapping helps dictate surgical approaches and fixation strategies.
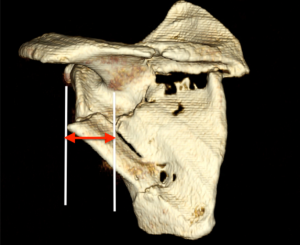
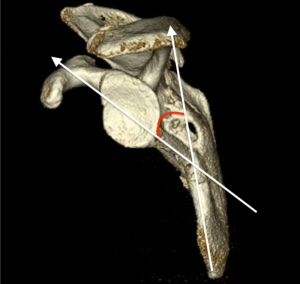
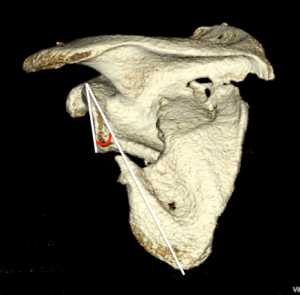
Current radiographic parameters indicating surgical fixation of scapular body fractures include lateral border offset (LBO), angulation, and glenopolar angle (GPA). LBO refers to the amount of displacement of the glenoid component in relation to the lateral border of the scapula. As described by Anavian et al. (6), this is found by measuring the distance between vertical lines drawn from the superolateral tip of the lateral border fracture inferiorly and its corresponding fracture bed at the base of the scapular neck superiorly, as seen on an AP radiograph or three-dimensional CT scan (Figure 2). Angulation of scapular body fractures is best determined on a scapular Y view by measuring the angle formed between parallel lines drawn down the proximal and distal segment cortices (6) (Figure 3). Finally, the GPA refers to the obliquity of the glenoid in respect to the scapular body (12). It is formed by first drawing a line from the superior point of the glenoid cavity to the inferior aspect compared with a second line drawn from the superior point of the glenoid to the inferior angle of the scapula body (6) (Figure 4).
Nonoperative treatment
Scapula fractures have classically been treated without surgery. Research has shown successful outcomes with this strategy (13-19). The usual treatment is a sling for about 3 weeks to allow subsidence of pain and swelling. During this time, close vigilance is important, as some patients with extraarticular variants were found to develop increasing deformity in the first weeks of treatment (20). Because of the unique anatomy of the periscapular region, many factors can lead to increased displacement and deformity, such as gravity, asymmetric muscle contractions, and fracture instability. Deforming forces can result in displacement, leading to pain, weakness and glenohumeral imbalance (12,14,15,21,22). Patients must therefore be monitored radiographically to detect early displacement and deformity. Because the scapula is 30 degrees off the plane of the thorax, fractures can be easily missed even in experienced centers (23,24).
The rehabilitation process is an important component regardless of treatment choice. It is important to keep in mind that patients may develop pseudoparalysis and dyskinesia in the early stages of rehabilitation. Additionally, treating surgeons must be aware that these injuries tend to be the result of high energy trauma, and associated injuries to the limb and chest wall must be addressed and accounted for in the rehabilitation process. Associated injuries are reported in up to 90% of cases and can serve as distracting injuries to prompt diagnosis.
Surgical treatment
The scapula is an integral part of the superior shoulder suspensory mechanism, which attaches the upper extremity to the axial skeleton. Seventeen muscular attachments and insertions provide a robust platform from which glenohumeral motion occurs (25). In the setting of a fracture, these can also be sources of deformity and displacement. The levator scapulae muscle, which inserts on the superomedial border of the scapula can medialize the cranial fragment but most commonly the lateral border is translated laterally by its attached musculature. This can be correlated radiographically as LBO and decreased GPA. Posterior surgical approaches are generally safe in regards to vascularity, since the subscapularis muscle originates from the anterior surface of the scapula and provides the blood supply to fracture fragments. The acromion and clavicle serve as the origin for the deltoid muscle. The lateral border of the scapula is the origin of the teres major and minor muscles, as well as the insertion point for the long head of the triceps and provides the most important bony fixation point for stable internal fixation.
As with all operations in orthopedic surgery, the surgical approach is of utmost importance in order to access the area of interest and apply hardware safely. The classic Judet approach is an extensile approach and exposes the entire posterior scapula by elevating the infraspinatus and teres minor, but this is rarely necessary for acute extraarticular fractures (1). Typically, the Judet curvilinear skin incision is utilized and muscular intervals are exploited for fracture reduction and fixation with less soft tissue disruption (26).
Depending on the fracture pattern, different intermuscular windows can be employed. A more limited technique can be used to access portions of the lateral border, scapular spine, and vertebral border. To do this, the muscle plane entered at the spine of the scapula is between the trapezius, originating at the superior margin, and the deltoid at the inferior margin, which is elevated (27,28). The majority of extraarticular fractures can be accessed with little or no release of the deltoid, but the medial portion of the deltoid origin can be released if needed and later repaired.
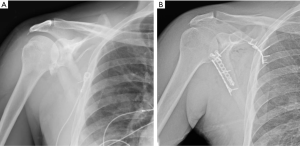
The acromion can be accessed with an extension of the posterior Judet incision laterally along the posterior acromion. At the vertebral border of the scapula, the intramuscular plane is between the infraspinatus which is elevated, and the rhomboids, which are left attached. The most important window is between the infraspinatus and teres minor for access to the lateral border of the scapula and the posterior glenoid rim. Once this interval is developed, the lateral border of the scapula can be exposed. This is a critical location for fracture reduction, which is typically anteversion of the glenoid and medialization of the lateral border fragment. Once reduced, typical fixation consists of low-profile, relatively flexible implants (Figure 5), such as 2.7 mm locking compression or reconstruction plates.
Outcomes
The surgical treatment of extraarticular scapular fractures remains controversial due to the acceptable results of nonoperative treatment and the lack of high-quality evidence comparing operative to nonoperative treatment. However, not all extraarticular scapular fractures can uniformly be treated nonoperatively with reproducibly excellent clinical outcomes.
Nonoperative treatment of minimally displaced scapular body fractures can reliably produce acceptable clinical results. Numerous authors (15,16,29,30) have published case series regarding the efficacy of nonoperative treatment of such fractures. In a recent retrospective case series of nonoperatively treated scapular body fractures, Gosens et al. (30) demonstrated functional shoulder scores equal to the general population. Nordqvist (14) in an earlier retrospective case series of scapular body, neck, or spine fractures found those with less than a centimeter of displacement largely had normal function when evaluated 10 to 20 years later. Some patients did experience a 25–50% reduction in range of motion in the affected shoulder (14). A subset of patients with displaced scapular neck fractures had poorer outcomes, an observation that was duplicated by Ada and Miller (10).
Subsequently, numerous reports of scapular neck malunions leading to increased shoulder dysfunction surfaced. Romero et al. (12) published a series focusing on malalignment of the glenoid neck marked by a severely decreased GPA. They found that those with a GPA <20 degrees had significantly increased pain, reduced activities of daily living, and abduction weakness at long-term follow-up (12). Bozkurt (15) and Kim (31) published similar findings that correlated a decreased GPA with worse Constant scores at follow-up. Glenopolar <20 degrees remain the relative surgical indication with the largest body of literature support.
The literature has demonstrated that operatively treated scapular body fractures consistently regain preoperative shoulder function at the expense of associated surgical complications. In one of the earlier operative series, Hardegger (4) reported on 33 surgical patients of which 64% returned to normal function while experiencing two infections and two hematomas requiring evacuation. In the largest recent retrospective surgical series of extraarticular scapula fractures by Schroder (32), the mean DASH score was comparable to standard population norms while strength and range of motion were comparable to the contralateral shoulder. The complication rate or secondary surgery rate in this series was 16% (32). In a retrospective matched cohort of 31 nonoperative and operative scapular fractures performed by Jones (5), the final range of motion of both groups was similar and no difference was found in return to work, pain, or complications. A selection bias did occur as those who received surgery had significantly more displacement than those who were treated nonoperatively (5). There were no complications related to scapular osteosynthesis in his series (5).
Conclusions
The management of extraarticular scapular fractures remains controversial due to the lack of prospective, randomized controlled trials justifying surgical intervention. Plain radiographs with evidence of scapular displacement should warrant a CT scan with 3D reconstruction, paying careful attention to LBO, angulation, and the GPA.
In general, the majority of scapula fractures can successfully be treated nonoperatively with excellent functional results. However, numerous case studies exist demonstrating poor outcomes of scapular body or neck fractures with increased deformity (12,14,15). The literature suggests that a GPA less than 20 degrees can lead to significantly worse shoulder function (12,15,30). Additionally, retrospective studies using LBO greater than >2 cm and angulation >45 degrees as a surgical indication demonstrate functional outcomes with near normal strength and range of motion and low complication rates. While numerous cut-offs for surgical indications have been recommended (5,33,34), all indications are considered relative and treatment should be individualized based on patient characteristics and goals.
Should we be fixing more of these? Perhaps, but more importantly, we should be diagnosing more of these and presenting our patients with all of their treatment options, surgical and non-surgical.
Acknowledgments
The authors would like to give special thanks to Lavi Mattingly for his tireless work editing and formatting this article for publication.
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned by the Guest Editor (Adam Seidl) for the series “Management of Fractures Around the Shoulder” published in Annals of Joint. The article has undergone external peer review.
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/aoj-20-46). The series ““Management of Fractures Around the Shoulder” was commissioned by the editorial office without any funding or sponsorship. PAC reports grants from Stryker, grants from Depuy-Synthes, other from KLS Martin, grants from AONA, COTA, OMeGA Depuy-Synthes, Stryker, Zimmer-Biomet, BoneFoam, Acumed, KLSMartin, Exactech, other from BoneFoam, personal fees from Exactech, Depuy-Synthes, personal fees from AO International, outside the submitted work. The authors have no other conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Judet R. Surgical Treatment of Scapular Fractures. Acta Orthop Belg 1964;30:673-8. [PubMed]
- Rowe CR. Fractures of the Scapula. Surg Clin North Am 1963;43:1565-71. [Crossref] [PubMed]
- Schnepp J, Comtet JJ, Cetre J, et al. Value of nonsurgical treatment of omoplata fractures. Lyon Med 1968;220:809-13. [PubMed]
- Hardegger FH, Simpson LA, Weber BG. The operative treatment of scapular fractures. J Bone Joint Surg Br 1984;66:725-31. [Crossref] [PubMed]
- Jones CB, Sietsema DL. Analysis of operative versus nonoperative treatment of displaced scapular fractures. Clin Orthop Relat Res 2011;469:3379-89. [Crossref] [PubMed]
- Anavian J, Conflitti JM, Khanna G, et al. A reliable radiographic measurement technique for extra-articular scapular fractures. Clin Orthop Relat Res 2011;469:3371-8. [Crossref] [PubMed]
- Armitage BM, Wijdicks CA, Tarkin IS, et al. Mapping of scapular fractures with three-dimensional computed tomography. J Bone Joint Surg Am 2009;91:2222-8. [Crossref] [PubMed]
- Cole PA, Gauger EM, Schroder LK. Management of scapular fractures. J Am Acad Orthop Surg 2012;20:130-41. [Crossref] [PubMed]
- Yadav V, Khare GN, Singh S, et al. A prospective study comparing conservative with operative treatment in patients with a 'floating shoulder' including assessment of the prognostic value of the glenopolar angle. Bone Joint J 2013;95-B:815-9. [Crossref] [PubMed]
- Ada JR, Miller ME. Scapular fractures. Analysis of 113 cases. Clin Orthop Relat Res 1991;174-80. [PubMed]
- Meinberg EG, Agel J, Roberts CS, et al. Fracture and Dislocation Classification Compendium-2018. J Orthop Trauma 2018;32:S1-170. [Crossref] [PubMed]
- Romero J, Schai P, Imhoff AB. Scapular neck fracture--the influence of permanent malalignment of the glenoid neck on clinical outcome. Arch Orthop Trauma Surg 2001;121:313-6. [Crossref] [PubMed]
- McGinnis M, Denton JR. Fractures of the scapula: a retrospective study of 40 fractured scapulae. J Trauma 1989;29:1488-93. [Crossref] [PubMed]
- Nordqvist A, Petersson C. Fracture of the body, neck, or spine of the scapula. A long-term follow-up study. Clin Orthop Relat Res 1992;139-44. [Crossref] [PubMed]
- Bozkurt M, Can F, Kirdemir V, et al. Conservative treatment of scapular neck fracture: the effect of stability and glenopolar angle on clinical outcome. Injury 2005;36:1176-81. [Crossref] [PubMed]
- Wilber MC, Evans EB. Fractures of the scapula. An analysis of forty cases and a review of the literature. J Bone Joint Surg Am 1977;59:358-62. [Crossref] [PubMed]
- Oh W, Jeon IH, Kyung S, et al. The treatment of double disruption of the superior shoulder suspensory complex. Int Orthop 2002;26:145-9. [Crossref] [PubMed]
- Schofer MD, Sehrt AC, Timmesfeld N, et al. Fractures of the scapula: long-term results after conservative treatment. Arch Orthop Trauma Surg 2009;129:1511-9. [Crossref] [PubMed]
- van Noort A, van Kampen A. Fractures of the scapula surgical neck: outcome after conservative treatment in 13 cases. Arch Orthop Trauma Surg 2005;125:696-700. [Crossref] [PubMed]
- Anavian J, Khanna G, Plocher EK, et al. Progressive displacement of scapula fractures. J Trauma 2010;69:156-61. [Crossref] [PubMed]
- Chadwick EK, van Noort A, van der Helm FC. Biomechanical analysis of scapular neck malunion--a simulation study. Clin Biomech (Bristol, Avon) 2004;19:906-12. [Crossref] [PubMed]
- Pace AM, Stuart R, Brownlow H. Outcome of glenoid neck fractures. J Shoulder Elbow Surg 2005;14:585-90. [Crossref] [PubMed]
- Herrera DA, Anavian J, Tarkin IS, et al. Delayed operative management of fractures of the scapula. J Bone Joint Surg Br 2009;91:619-26. [Crossref] [PubMed]
- Tadros AM, Lunsjo K, Czechowski J, et al. Causes of delayed diagnosis of scapular fractures. Injury 2008;39:314-8. [Crossref] [PubMed]
- van der Helm FC, Pronk GM. Three-dimensional recording and description of motions of the shoulder mechanism. J Biomech Eng 1995;117:27-40. [Crossref] [PubMed]
- Obremskey WT, Lyman JR. A modified Judet approach to the scapula. J Orthop Trauma 2004;18:696-9. [Crossref] [PubMed]
- Braun C, Wirbel R, Mutschler W. The two-portal approach for internal fixation of scapular fractures. Eur J Trauma 2005;31:186-93. [Crossref]
- Gauger EM, Cole PA. Surgical technique: a minimally invasive approach to scapula neck and body fractures. Clin Orthop Relat Res 2011;469:3390-9. [Crossref] [PubMed]
- Edwards SG, Whittle AP, Wood GW 2nd. Nonoperative treatment of ipsilateral fractures of the scapula and clavicle. J Bone Joint Surg Am 2000;82:774-80. [Crossref] [PubMed]
- Gosens T, Speigner B, Minekus J. Fracture of the scapular body: functional outcome after conservative treatment. J Shoulder Elbow Surg 2009;18:443-8. [Crossref] [PubMed]
- Kim KC, Rhee KJ, Shin HD, et al. Can the glenopolar angle be used to predict outcome and treatment of the floating shoulder? J Trauma 2008;64:174-8. [Crossref] [PubMed]
- Schroder LK, Gauger EM, Gilbertson JA, et al. Functional outcomes after operative management of extra-articular glenoid neck and scapular body fractures. J Bone Joint Surg Am 2016;98:1623-30. [Crossref] [PubMed]
- Cole PA, Gauger EM, Herrera DA, et al. Radiographic follow-up of 84 operatively treated scapula neck and body fractures. Injury 2012;43:327-33. [Crossref] [PubMed]
- Jones CB, Cornelius JP, Sietsema DL, et al. Modified Judet approach and minifragment fixation of scapular body and glenoid neck fractures. J Orthop Trauma 2009;23:558-64. [Crossref] [PubMed]
Cite this article as: Heare A, Oleszkiewicz SM, Irizarry RCH, Cole PA. Scapular body fractures—should we be fixing more of these? Ann Joint 2021;6:22.


