The burden of prosthetic joint infection (PJI)
Total hip and knee arthroplasty are clinically and cost effective procedures. The numbers of patients receiving these procedures are estimated to rise by 150–600% for THA and TKA respectively by 2030 (1) in the USA. The trend is similar in Europe (2,3). Along with this trend in hip and knee arthroplasty patients increasingly also have indwelling prostheses of the shoulder, elbow and ankle.
Prosthetic joint infection (PJI) is potentially the most significant complication following total joint arthroplasty. It is challenging for the surgeon to manage, physically and mentally disastrous for the patient and the cost to the health care system and society as a whole is high. PJI has an impact on patients, healthcare delivery institutions and society as a whole. It has significant negative impact on patients’ psychological well being (4). The cost of treating PJI is significant. It is estimated that in the US alone the projected spend on the treatment of PJI is $1.62 billion (5). This is despite little improvement in the success rate in terms of eradication of infection (6).
For these reasons there has been an increasing focus on the issue of PJI in the medical literature (6). This paper discusses the incidence of PJI as well as the factors which might account for the current trends and the challenges associated with the contemporary management of PJI.
The incidence of PJI varies with the joint involved (7,8). Reported incidences following total knee arthroplasty, total hip arthroplasty and total shoulder arthroplasty have been reported to be 0.25% to 2%, 0.5% to 1% and less than 1% respectively (9,10). Between 23–25% of revision TKA procedures and 12–15% revision THA procedures are performed for PJI (11,12). Risk factors for PJI are presented in Table 1 (13). While the incidence remains low the number of patients are likely to increase over time however as the number of arthroplasty procedures performed annually increases.

Full table
The incidence of PJI varies throughout the literature. As a result existing data needs to be interpreted with caution. Wang et al. (14) reported a reduction in the incidence of PJI from 1.9% to 0.76% between 2006 and 2014. Likewise, Runner and colleagues (15) reported a reduction in the incidence of PJI from 1.4% to 0.6% between 2008 and 2016. This is at variance with reports from the United States National Inpatient Sample suggesting that between 2001 and 2009 the incidence of PJI in patients having THA increased from 1.99% to 2.18% and 2.05% to 2.18% for patients having TKA (16). Data from the Nordic Arthroplasty Registry has reported an increase in the rate of revision procedures performed for infected THA from 0.46% to 0.71% between 1999 and 2009 (17). Infection is still represented among the five most common indications for revision surgery in all major joint registries. What is clear from the existing literature is that the numbers of total hip and knee arthroplasties are increasing annually. The frequency of these procedures translates a relatively low incidence into a substantial burden of PJI faced by practising clinicians and institutions. What is less controversial is that the physiologic status of patients presenting for total joint arthroplasty is changing. The percentage of patients recorded as American Society of Anaesthesiologists (ASA) Class 1 (fit and healthy) has decreased from 16% to 12% between 2010 and 2018. Over the same period the number of patients classified as ASA Class 3 (incapacitating systemic disease) has increased from 15% to 20% over the same period (18).
PJI is becoming an increasingly important issue in the discipline of reconstructive orthopaedics. The associated 90 day mortality rate is approximately 4% compared to 0.3% combined mortality rate following primary total hip and knee arthroplasty (19).
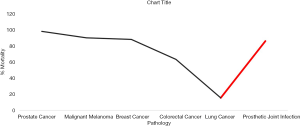
Mortality rates associated with PJI are significant and concerning. Twenty four percent to 26% mortality has been reported for patients with PJI of the hip. Parvizi and colleagues found significant differences in mortality rates in patients undergoing revision for PJI compared to aseptic loosening at 30–90 days (3.7% vs. 0.8%) and 90 days to 1 year (10.6% vs. 2%). The mortality rates for PJI is comparable to breast cancer and higher than that for colorectal and lung cancer (20) (Figure 1).
This special series focuses on the increasingly important issue of PJI. We present expert reviews of the contemporary and important topics and attempt to shed some clarity on the controversial aspects of management of PJI. We illustrate why this issue is rightly a growing concern in contemporary orthopaedic practice across the globe.
Acknowledgments
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned by the editorial office, Annals of Joint for the series “Prosthetic Joint Infection”. The article did not undergo external peer review.
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/aoj-2020-pji-11). The series “Prosthetic Joint Infection” was commissioned by the editorial office without any funding or sponsorship. MAS, MF and DK served as the unpaid Guest Editors of the series. The authors have no other conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Kurtz S, Ong K, Lau E, et al. Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Am 2007;89:780-5. [Crossref] [PubMed]
- Leitner L, Türk S, Heidinger M, et al. Trends and Economic Impact of Hip and Knee Arthroplasty in Central Europe: Findings from the Austrian National Database. Sci Rep 2018;8:4707. [Crossref] [PubMed]
- Robertsson O, Bizjajeva S, Fenstad AM, et al. Knee arthroplasty in Denmark, Norway and Sweden. A pilot study from the Nordic Arthroplasty Register Association. Acta Orthop 2010;81:82-9. [Crossref] [PubMed]
- Moore AJ, Blom AW, Whitehouse MR, et al. Deep prosthetic joint infection: a qualitative study of the impact on patients and their experiences of revision surgery. BMJ Open 2015;5:e009495 [Crossref] [PubMed]
- Haddad FS, Ngu A, Negus JJ. Prosthetic Joint Infections and Cost Analysis? Adv Exp Med Biol 2017;971:93-100. [Crossref] [PubMed]
- Sandiford NA, McHale A, Citak M, et al. What is the optimal duration of intravenous antibiotics following single-stage revision total hip arthroplasty for prosthetic joint infection? A systematic review. Hip Int 2021;31:286-94. [Crossref] [PubMed]
- Beam E, Osmon D. Prosthetic Joint Infection Update. Infect Dis Clin North Am 2018;32:843-59. [Crossref] [PubMed]
- Koh CK, Zeng I, Ravi S, et al. Periprosthetic joint infection is the main cause of failure for modern knee arthroplasty: an analysis of 11,134 knees. Clin Orthop Relat Res 2017;475:2194-201. [Crossref] [PubMed]
- Namba RS, Inacio MC, Paxton EW. Risk factors associated with deep surgical site infections after primary total knee arthroplasty: an analysis of 56,216 knees. J Bone Joint Surg Am 2013;95:775-82. [Crossref] [PubMed]
- Edwards JR, Peterson KD, Mu Y, et al. National Healthcare Safety Network (NHSN) report: data summary for 2006 through 2008, issued December 2009. Am J Infect Control 2009;37:783-805. [Crossref] [PubMed]
- Bozic KJ, Kurtz SM, Lau E, et al. The epidemiology of revision total knee arthroplasty in the United States. Clin Orthop Relat Res 2010;468:45-51. [Crossref] [PubMed]
- National Joint Registry for England and Wales. Available online: http://www.njrcentre.org.uk/NjrCentre/Portals/0/Documents/England/Reports/9th_annual_report/NJR%209th%20Annual%20Report%202012.pdf (Accessed 5/7/2020).
- Lenguerrand E, Whitehouse MR, Blom AW. Risk factors associated with revision for prosthetic joint infection after knee replacement - Authors’ reply. Lancet Infect Dis 2019;19:807-8. [Crossref] [PubMed]
- Wang FD, Wang YP, Chen CF, et al. The incidence rate, trend and microbiological aetiology of prosthetic joint infection after total knee arthroplasty: A 13 years’ experience from a tertiary medical center in Taiwan. J Microbiol Immunol Infect 2018;51:717-22. [Crossref] [PubMed]
- Runner RP, Mener A, Roberson JR, et al. Prosthetic Joint Infection Trends at a Dedicated Orthopaedics Specialty Hospital. Adv Orthop 2019;2019:4629503 [Crossref] [PubMed]
- Kurtz SM, Lau E, Watson H, et al. Economic burden of periprosthetic joint infection in the United States. J Arthroplasty 2012;27:61-5.e1.
- Dale H, Fenstad AM, Hallan G, et al. Increasing risk of prosthetic joint infection after total hip arthroplasty. Acta Orthop 2012;83:449-58.
- National Joint Registry for England and Wales. Available online: https://reports.njrcentre.org.uk/hips-primary-procedures-patient-characteristics/H09v2NJR?reportid=F2DDCB30-DF06-4432-B183-E591FE71BEE6&defaults=DC__Reporting_Period__Date_Range=%22MAX%22,H__JYS__Filter__Calendar_Year__From__To=%22min-max%22,H__Filter__Joint=%22Hip%22 (Accessed 14/7/2020).
- Jorgensen CC., Kehlet H. Time course and reasons for 90-day mortality in fast-track hip and knee arthroplasty. Acta Anaesthesiol Scand 2017;61:436-44.
- Parvizi J and Zmistowski B. A quarter of patients treated for PJI dead within 5 years. Available online: https://www.healio.com/news/orthopedics/20130104/a-quarter-of-patients-treated-for-pji-dead-within-5-years, accessed 14-7-2020.
Cite this article as: Sandiford NA, Francescini M, Kendoff D. The burden of prosthetic joint infection (PJI). Ann Joint 2021;6:25.